The Two Problems That Look the Same — But Aren’t
There is a moment in clinical medicine that almost every provider recognizes.
The patient is struggling to breathe.
Their chest rises and falls quickly.
Maybe their shoulders are lifting with each breath.
Maybe they are sitting upright, leaning forward, searching for air.
You can feel the tension in the room.
Someone reaches for the oxygen mask.
And someone inevitably says:
“Put oxygen on them.”
It is one of the most deeply ingrained reflexes in medicine.
Breathing problem?
Give oxygen.
And to be fair, that instinct has saved countless lives.
But here is the uncomfortable truth.
Respiratory distress is not a diagnosis.
It is a symptom.
And sometimes the physiology hiding behind that symptom has very little to do with oxygen at all.
In fact, there are two completely different physiological failures that can produce the same terrifying image of a patient struggling to breathe.
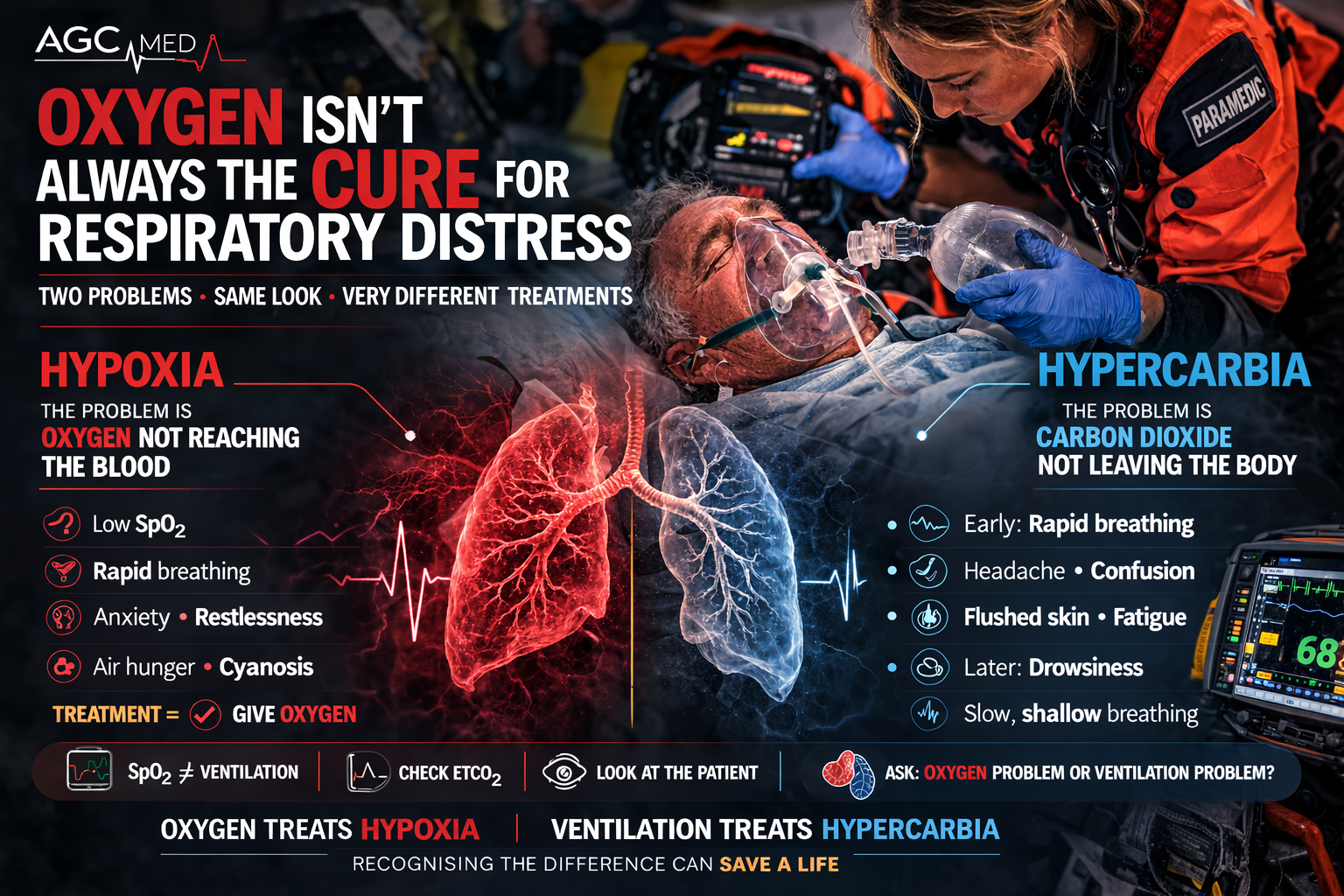
One is hypoxia.
The other is hypercarbia.
They look similar at the bedside.
They sound similar in conversation.
But they represent two fundamentally different problems inside the body — and they demand two very different treatments.
Understanding the difference is one of the most important skills clinicians develop over time.
Because sometimes the mask helps.
And sometimes the mask hides the real problem entirely.
The Two Jobs of the Lungs
The lungs perform two critical physiological tasks.
They bring oxygen into the body.
And they remove carbon dioxide from the body.
These two processes are related, but they are not the same.
Oxygenation
The transfer of oxygen from the alveoli into the bloodstream.
Ventilation
The movement of air in and out of the lungs to eliminate carbon dioxide.
In everyday conversation these terms are often used interchangeably.
But physiologically they are separate processes with separate failure modes [1].
A patient can fail at oxygenation.
A patient can fail at ventilation.
Or sometimes, both can occur at the same time.
But the distinction matters.
Because the treatment for one problem does not necessarily treat the other.
Hypoxia: When Oxygen Cannot Reach the Blood
Hypoxia occurs when tissues do not receive enough oxygen to support normal cellular metabolism [2].
In this situation, the bloodstream itself becomes poorly oxygenated.
The lungs may be moving air.
But oxygen is not effectively transferring from the alveoli into the blood.
There are many reasons this can happen.
Fluid may fill the alveoli, as seen in pulmonary edema.
Inflammation may damage the alveolar membrane, as seen in ARDS.
Infection may impair gas exchange, as seen in pneumonia.
Blood flow may bypass ventilated alveoli, as seen with pulmonary embolism.
Or the oxygen content of the air itself may be reduced, as occurs at high altitude.
In each of these situations the lungs are still moving air.
But oxygen cannot effectively reach the bloodstream.
The body senses this quickly.
Peripheral chemoreceptors located in the carotid and aortic bodies detect falling oxygen tension and stimulate an increase in respiratory effort [3].
The patient begins to breathe faster.
Harder.
Deeper.
Clinically, hypoxic patients often appear:
• Tachypneic
• Restless
• Anxious
• Air hungry
And in severe cases:
• Cyanotic
• Confused
• Hypotensive
In these patients oxygen therapy addresses the underlying physiology directly.
Increasing the concentration of oxygen in the alveoli increases the gradient driving diffusion into the bloodstream [4].
Sometimes a nasal cannula is sufficient.
Sometimes patients require more aggressive support:
• Non-rebreather masks
• High-flow nasal oxygen
• CPAP
• Mechanical ventilation
In hypoxia the equation is simple.
The body lacks oxygen.
So we provide oxygen.
Hypercarbia: When Carbon Dioxide Cannot Leave
Hypercarbia — more precisely called hypercapnia — is a completely different physiological failure.
In this scenario oxygen may still be entering the bloodstream normally.
The problem lies elsewhere.
Carbon dioxide is not leaving the body.
Carbon dioxide is produced continuously by cellular metabolism.
Every minute the body must eliminate this waste gas through ventilation [1].
When ventilation becomes inadequate, carbon dioxide accumulates.
PaCO₂ rises.
Blood pH begins to fall.
Respiratory acidosis develops [5].
This process can occur for many reasons.
The brain may fail to drive breathing, as seen in opioid overdose or brainstem injury.
The respiratory muscles may fail, as seen in neuromuscular disease.
Airflow obstruction may limit effective ventilation, as seen in COPD or severe asthma.
Or the patient may simply become too exhausted to sustain the work of breathing.
One of the most common misconceptions in respiratory medicine is that hypercapnia presents with slow breathing.
In reality the opposite is often true.
Early hypercarbia usually produces rapid breathing.
Rising carbon dioxide stimulates central chemoreceptors within the medulla, increasing respiratory drive through changes in cerebrospinal fluid pH [3].
The patient attempts to compensate by breathing faster.
Harder.
Deeper.
But if ventilation remains ineffective, carbon dioxide continues to rise.
As hypercapnia worsens the clinical picture begins to change.
Patients may develop:
• Headache
• Confusion
• Flushed skin
• Agitation
Eventually the brain itself becomes affected by rising CO₂ levels.
The patient becomes drowsy.
Respiratory effort begins to decline.
CO₂ narcosis develops [6].
And unless ventilation is restored, respiratory arrest follows.
And here lies the critical lesson.
Oxygen does not remove carbon dioxide.
A hypercarbic patient can receive high-flow oxygen and still deteriorate if ventilation remains inadequate [7].
The solution to hypercarbia is not simply oxygen.
The solution is ventilation.
When the Monitor Lies
One of the most dangerous moments in respiratory care occurs when the monitor reassures us.
Consider a patient with opioid-induced hypoventilation.
Their oxygen saturation may initially appear normal.
Yet their ventilation is slowing.
Carbon dioxide is rising.
Administering oxygen may maintain a reassuring SpO₂ reading while the patient becomes progressively more acidotic and less responsive [8].
The numbers look fine.
The physiology is not.
This is why clinicians must remember a simple but powerful rule.
Pulse oximetry measures oxygenation.
It does not measure ventilation. [9]
A patient can have a perfectly normal oxygen saturation while developing life-threatening hypercapnia.
How to Tell the Difference in 30 Seconds
When confronted with respiratory distress, clinicians can rapidly assess the underlying physiology.
Look at the oxygen saturation
Low SpO₂ suggests oxygenation failure.
Think pneumonia, pulmonary edema, ARDS, or pulmonary embolism.
Look at the breathing pattern
Rapid breathing may occur in both conditions.
But slow, shallow, ineffective breathing strongly suggests ventilation failure.
Use capnography
End-tidal CO₂ monitoring provides real-time insight into ventilation.
Rising EtCO₂ often signals ventilatory failure before oxygen saturation begins to fall [10].
Look at the patient
Hypoxic patients often appear desperate for air.
Hypercarbic patients often appear fatigued or progressively drowsy.
One looks like they cannot get oxygen in.
The other looks like they cannot move air out.
The Moment Every Paramedic Recognizes
Most experienced clinicians have seen this moment.
A patient in respiratory distress.
Their chest moves.
But the breaths are shallow.
You place the pulse oximeter.
SpO₂: 98%.
Someone says:
“His oxygen is fine.”
But the patient is becoming quieter.
Less responsive.
Something is wrong.
You place the capnography.
EtCO₂: 68 mmHg.
The problem was never oxygen.
The problem was carbon dioxide.
And unless someone recognizes that quickly, the next steps are predictable.
Acidosis.
Loss of airway reflexes.
Respiratory arrest.
For those who have witnessed it, the lesson never fades.
Respiratory distress is not always about oxygen.
Sometimes the patient simply needs help moving air.
Final Thoughts
Respiratory distress is one of the most urgent situations clinicians encounter.
The instinct to reach for oxygen is understandable.
But the best clinicians pause for a moment and ask a different question.
Is the patient lacking oxygen?
Or are they failing to ventilate?
Because oxygen treats hypoxia.
Ventilation treats hypercarbia.
And recognizing the difference can change everything.
References
-
West JB. Respiratory Physiology: The Essentials. 11th ed. 2021.
-
Martin L, Grocott MP. Oxygen therapy in critical illness. BMJ.
-
Hall JE. Guyton and Hall Textbook of Medical Physiology. 14th ed.
-
Tobin MJ. Principles and Practice of Mechanical Ventilation.
-
Lumb AB. Nunn’s Applied Respiratory Physiology.
-
Roussos C, Koutsoukou A. Respiratory failure. European Respiratory Journal.
-
O’Driscoll BR et al. Oxygen use in emergency settings. Thorax.
-
Boyer EW. Management of opioid overdose. NEJM.
-
Jubran A. Pulse oximetry. Critical Care.
-
Kodali BS. Capnography outside the operating room. Anesthesiology.