Introduction
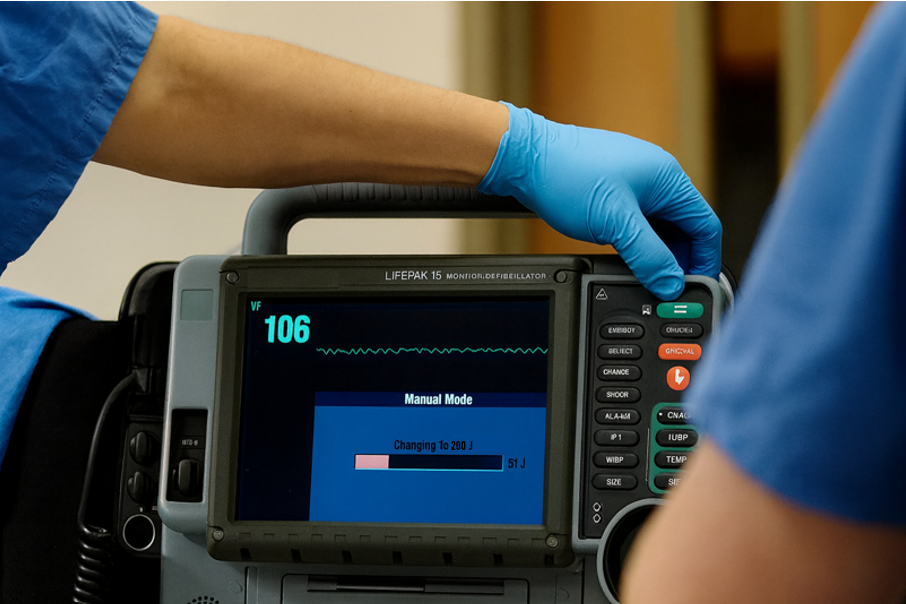
Shock-refractory ventricular fibrillation (VF) and pulseless ventricular tachycardia (pVT) remain among the most difficult cardiac arrest rhythms to manage. Even with rapid defibrillation and high-quality CPR, some patients simply don’t respond. The question has long been: can antiarrhythmic drugs like amiodarone or lidocaine improve outcomes once standard measures fail?
The landmark ALPS Trial (Amiodarone, Lidocaine, or Placebo Study) sought to answer exactly that — in a large, real-world EMS setting [1].
Study Overview
The ALPS Trial, conducted by the Resuscitation Outcomes Consortium, enrolled adults with out-of-hospital cardiac arrest whose rhythm remained shockable after at least one defibrillation attempt [1].
Patients were randomized during active resuscitation to receive amiodarone, lidocaine, or placebo alongside standard ACLS therapy.
Dosing reflected current practice:
-
Amiodarone: 300 mg IV/IO initial, followed by 150 mg if VF/pVT persisted [2].
-
Lidocaine: 120 mg IV/IO initial, followed by 60 mg if required [2].
The primary endpoint was survival to hospital discharge, with a key secondary outcome of favorable neurological status [2].
Key Results
1. Overall Survival
ALPS showed no statistically significant difference in survival to discharge between the three groups [3]:
-
Amiodarone ≈ 24.4%
-
Lidocaine ≈ 23.7%
-
Placebo ≈ 21.0%
Neurologically intact survival was also similar.
In short, antiarrhythmics did not increase overall survival when given after multiple failed shocks [3].
2. Subgroup Signals
When researchers analyzed only bystander-witnessed arrests, both amiodarone and lidocaine were associated with higher survival rates than placebo [3].
This suggests that when downtime is short and high-quality CPR is in progress, antiarrhythmics may add marginal benefit. In unwitnessed or prolonged arrests, the effect largely disappears.
3. Route of Administration: IV vs IO
A prespecified analysis looked at whether drug delivery route influenced outcomes [4].
Of 3,019 patients with known access, 2,358 received medication IV and 661 IO.
Results were revealing:
-
IV Amiodarone improved survival to discharge compared with placebo (adjusted +5.5%).
-
IV Lidocaine also improved survival (adjusted +4.7%).
-
IO administration, however, showed no benefit for either drug.
Although not statistically powered to prove an interaction, the trend clearly favored IV over IO delivery [4].
4. Timing Matters
A secondary ALPS analysis explored how time-to-drug affected success [5].
The odds of return of spontaneous circulation (ROSC) dropped with every minute of delay, regardless of the drug used.
However, for amiodarone, early administration was associated with significantly higher ROSC rates — its benefit diminished rapidly as time passed [5].
Lidocaine’s effect appeared more stable but less pronounced [5].
Clinical Implications for EMS and Critical Care
-
CPR and Defibrillation Still Come First
Drugs can’t fix poor compressions or delayed shocks. ALPS confirms that the foundation of resuscitation remains mechanical and electrical, not pharmaceutical [6]. -
Prefer IV Access When Possible
If IV access can be obtained quickly, it is the route of choice. IO delivery may blunt drug efficacy, particularly for lipophilic agents like amiodarone [4]. -
Give It Early — or Not at All
Amiodarone’s benefit shrinks with every passing minute. If you can’t administer it within the first few cycles of refractory VF, the effect may already be lost [5]. -
Amiodarone vs Lidocaine?
In ALPS, neither drug was superior overall. Lidocaine may have fewer post-resuscitation hypotension issues, while amiodarone may suppress recurrent VF better. The best choice is the one you can give quickly and correctly within your local protocol [3]. -
Set Realistic Expectations
Even under ideal conditions, the survival improvement is modest — around 4–5% absolute difference. Antiarrhythmics should be seen as supportive adjuncts, not game changers [6].
Conclusion
The ALPS Trial reshaped how we view antiarrhythmic therapy in cardiac arrest.
It reminded us that no medication replaces good CPR, timely defibrillation, and effective teamwork.
If you’re going to use a drug for refractory VF, give it early, IV if possible, and within a system that already excels at the basics.
That’s where science meets street medicine — and where the small gains matter most.
References
-
Resuscitation Outcomes Consortium ALPS Trial Protocol.
-
Kudenchuk PJ et al. “Amiodarone, Lidocaine, or Placebo in Out-of-Hospital Cardiac Arrest.” N Engl J Med. 2016; 374: 1711–1722.
-
International Liaison Committee on Resuscitation (ILCOR) Consensus on Science and Treatment Recommendations, 2018 Update.
-
Daya MR et al. “Association of Route of Vascular Access with Survival in the ALPS Trial.” Circulation. 2020; 141: 1235–1246.
-
Kudenchuk PJ et al. “Timing of Antiarrhythmic Drug Administration and Outcomes in the ALPS Trial.” Resuscitation. 2022; 170: 55–63.
-
Core Advanced Cardiac Life Support Guidelines (AHA 2020): Part 6 – Advanced Cardiovascular Life Support.