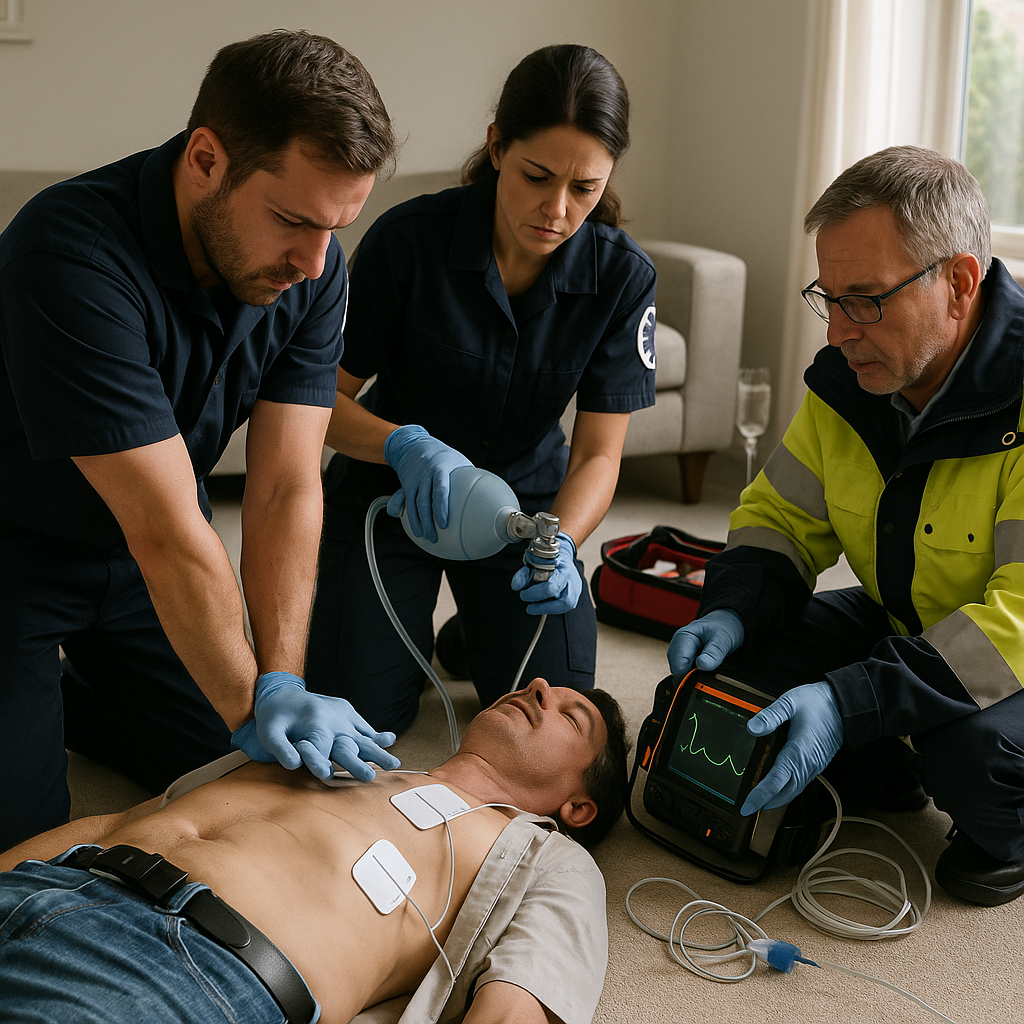
Introduction
When cardiac arrest happens, the natural instinct for many providers is to “load and go” — to rush the patient to the hospital, believing that definitive care lies beyond the walls of the emergency department. Yet, over the past two decades, data have increasingly challenged this reflex. The reality is that staying on scene and delivering high-quality CPR before considering transport offers patients a significantly higher chance of survival with good neurological outcomes.
Movement interrupts compressions. Shocks are delayed. Airway and vascular access become more difficult. The pit-crew coordination that drives effective resuscitation falls apart.
This article explores the science, physiology, and evidence behind the “stay and play” approach and highlights why resuscitation belongs at the scene, not en route.
Why “Stay, Don’t Go” Often Offers the Best Chance
1. Movement Inhibits Compressions
Even the most skilled providers cannot maintain consistent, guideline-quality compressions while an ambulance is in motion. Studies have shown that compression depth, rate, and recoil all deteriorate significantly when performed during transport. Moreover, the moments surrounding loading and departure are particularly damaging — often leading to prolonged “no-flow” intervals where perfusion is lost entirely.
Those lost minutes are costly. In cardiac arrest, every second of interrupted CPR translates to reduced coronary and cerebral perfusion and worse survival outcomes.
2. The First Minutes Are Crucial
The first few minutes after cardiac arrest represent a narrow physiologic window in which defibrillation and perfusion can restore organized cardiac activity. For every minute that passes without defibrillation, the chance of survival decreases by roughly 7–10%. Early shocks and uninterrupted compressions remain the single strongest predictors of neurologically intact survival. Delaying these interventions to move the patient is, in essence, delaying the only proven therapies that matter most in the early phase of cardiac arrest [1, 2].
3. Airway, Access, and Medications Are Easier On Scene
Advanced airway management, IV or IO access, and medication preparation are far safer and more reliable when performed on a stable, well-lit, and stationary scene. In a moving ambulance, providers face cramped space, vibration, and motion — all of which increase procedural errors and delay drug delivery. On scene, however, these interventions can be coordinated efficiently under calm, organized control [3].
4. The Pit-Crew Model Works
High-performance resuscitation teams operate like a Formula 1 pit crew — each member with a defined role, working in sync and with minimal interruptions. That choreography is nearly impossible to maintain in transit. Systems that have implemented this structured, on-scene pit-crew approach have consistently demonstrated higher rates of ROSC and neurologically intact discharge [4].
Evidence in Favor of On-Scene Resuscitation
While no randomized controlled trial can ethically assign patients to “stay” versus “go,” multiple large registry and propensity-matched studies support the superiority of on-scene resuscitation.
The Grunau et al. Study (JAMA 2020)
In a large multicenter cohort (n ≈ 27,700), survival to hospital discharge was 8.5% for patients who received continued on-scene resuscitation compared to just 4.0% for those transported during active CPR [1]. Neurologically favorable outcomes followed the same pattern (7.1% vs 2.9%). These findings remained consistent even after adjusting for confounders.
The conclusion was clear: early intra-arrest transport cuts survival in half.
Burns et al. (2023 Systematic Review)
A comparative review of expedited transport versus continued on-scene resuscitation found no survival advantage to rapid transport. In fact, moving patients before ROSC often correlated with lower rates of meaningful recovery [2].
Kim et al. (2025 National Multicenter Study)
A 2025 nationwide study examined the relationship between transport time interval (TTI) and on-scene CPR duration [3]. Patients with transport times ≥ 10 minutes had better neurologic outcomes when more time was spent on scene prior to transport (9.8% vs 7.4%). The optimal on-scene duration averaged about five minutes before considering movement, especially when hospitals were distant.
The takeaway: long transport times make immediate movement counterproductive.
Choi et al. (2024 Adaptive Model)
Choi and colleagues proposed a dynamic decision-making algorithm that uses real-time feedback to individualize when to transport versus when to continue on scene [4]. Their model confirmed what frontline providers already sense — that no single time threshold fits all cases, but a structured, data-driven approach can reduce unnecessary movement and improve outcomes.
Practical Decision Framework
From the evidence and physiologic understanding, a practical, field-ready framework emerges:
-
Prioritize CPR and defibrillation first. Early compressions and shocks remain the cornerstone of survival.
-
Estimate transport time early. If the hospital is far (>10 min), maximize on-scene resuscitation efforts.
-
Commit to a focused 5–10 minute on-scene window. Beyond that, reassess progress and potential reversibility.
-
Only move when transport adds something you can’t provide on scene. This includes cath-lab intervention, ECMO, or immediate access to advanced mechanical support [5].
-
Reassess continuously. If ROSC occurs, stabilize first, then package and transport safely.
-
Train and simulate the pit-crew model. Effective teamwork requires planning, repetition, and discipline.
Addressing Common Objections
“What about rural or remote systems?”
If transport time to definitive care is extreme and resources are limited, early movement may still be necessary. But even then, brief on-scene stabilization with defibrillation and airway control improves outcomes [6].
“What about patients who could benefit from ECMO or PCI?”
These are the key exceptions. If the patient arrests within close proximity to an ECMO-capable or PCI-capable center, rapid transport can be justified [7].
“Aren’t these just observational studies?”
Yes — but they are large, rigorously adjusted, and remarkably consistent in their conclusions: intra-arrest transport before ROSC almost always worsens survival.
Conclusion
In modern EMS, speed does not equal success. Moving the patient quickly may feel like action, but in cardiac arrest, movement often means interruption, chaos, and lost perfusion. Staying on scene allows focused, coordinated, high-quality resuscitation — the single most important determinant of survival.
Unless a reversible cause or advanced hospital therapy is immediately accessible, the evidence is clear:
Stay, work, shock, and reassess. Don’t move until the heart beats again.
This is how we give our patients the best chance not just to survive, but to walk out of the hospital neurologically intact.
References
-
Grunau B, Scheuermeyer FX, Stub D et al. Association of Intra-Arrest Transport vs Continued On-Scene Resuscitation with Survival to Hospital Discharge. JAMA. 2020; 324(11): 1058–1067.
-
Burns B et al. Expedited Transfer Versus Continued On-Scene Resuscitation in Out-of-Hospital Cardiac Arrest. Systematic Review, 2023.
-
Kim D, Yu JY, Kim M et al. Adjusting On-Scene CPR Duration Based on Transport Time Interval in Out-of-Hospital Cardiac Arrest: A Nationwide Multicenter Study. Scientific Reports, 2025.
-
Choi D et al. Individualized Decision-Making in On-Scene Resuscitation Time for Out-of-Hospital Cardiac Arrest. 2024.
-
de Graaf C et al. Time to Return of Spontaneous Circulation and Survival: When to Transport in Out-of-Hospital Cardiac Arrest. Reanimate Conference Monograph, 2022.
-
Burns B et al. Expedited Transfer from the Scene for Refractory Out-of-Hospital Cardiac Arrest. ScienceDirect, 2025.
-
American Heart Association. 2020 Guidelines for CPR and Emergency Cardiovascular Care: Part 3 – Adult Basic and Advanced Life Support.